“This morning I saw the countryside from my window a long time before sunrise, with nothing but the morning star, which looked very big”, writes Van Gogh in a letter to his brother, Theo. The famous oil-on-canvas painting ‘Starry Night’ was inspired by this view from the window of Saint-Paul-de-Mausole asylum in southern France where he spent the year 1889. He suffered from mental illness most of his life. Speculations still surround his comorbid mental illnesses. Clinicians attribute some of his extreme mood swings and dramatic behaviour to Bipolar Affective Disorder (BPAD), a neuropsychiatric illness that causes massive shifts in energy and mood shuttling between intense excitement– known as mania to deep depression.
BPAD is sixth on the charts of disability-causing diseases worldwide and there is a pressing need for effective treatments. Mood stabilizers are the go-to treatment to soothe a bipolar brain and allow a patient to conduct a relatively normal life. One such mood stabilizer is lithium. It is an extremely valuable tool for doctors to manage bipolar disorder. However, there is a problem; lithium treatment is effective for only about a third of patients with bipolar disorder. The remaining patients with bipolar disorder show limited or no response to lithium treatment. As of now, doctors do not understand the reason for this varied response to lithium. As a result, they are unable to choose the correct treatment for a bipolar patient when they are brought to the clinic for treatment. One of the reasons for this inability to predict the response of an individual to treatment is that we do not have a clear understanding of how lithium acts on the brain leading to an improvement in a patient’s condition.
In a recent study, published in Life Science Alliance, Raghu Padinjat and his group at NCBS have found an explanation to how lithium acts on brain cells to change neural activity. These findings can enable tailored approaches and the development of new treatments.
“To understand why some patients do not respond to lithium treatment, we need to know how lithium exerts its effects”, says Sankhanil Saha, lead author of the study.
In the brain, communication between cells leading to normal behaviour occurs through chemicals called neurotransmitters. These neurotransmitters, such as serotonin or glutamate bind to receptors on the neural cell membrane that switch on an enzyme called phospholipase C (PLC). The role of PLC is to break down a lipid molecule–phosphatidylinositol 4,5-bisphosphate (PIP2) into inositol 1,4,5-trisphosphate (IP3) which orchestrates changes in calcium levels within the cells. Calcium performs many functions within the brain and previous studies that altered calcium levels within neurons is a likely basis for bipolar disorder.
Lithium pacifies hyperactive neurons
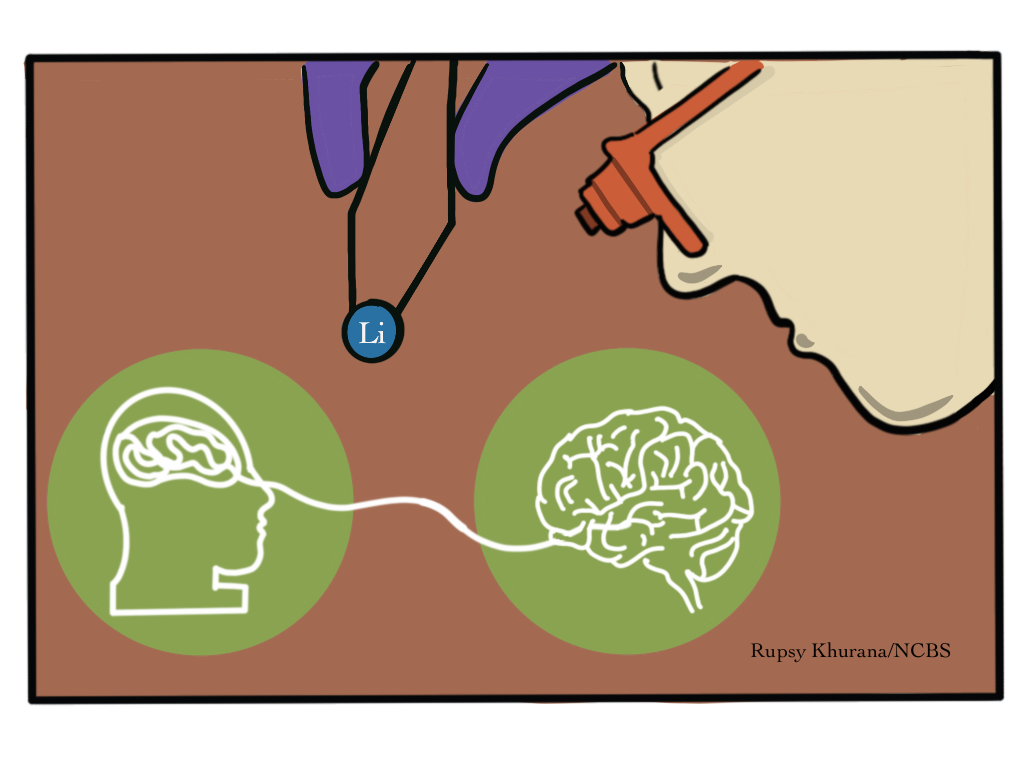
In individuals with BPAD, the PIP2 pathway is in hyperactive mode which leads to elevated calcium levels in the cell, says Sankhanil. To understand lithium’s stabilizing effect, they treated lab-grown cortical cells of the human forebrain with neurotransmitters to mimic the activity of a bipolar patient’s brain cells. This activated the PLC, mimicking the overstimulated cells of a bipolar brain. On adding lithium to the mix, the team observed a delay in the re-synthesis of PIP2. Consequently, it slowed down the formation of IP3 and reduced calcium influx that dampened the activity of neurons.
Raghu and team dug deeper to investigate how lithium delayed the PIP2 re-synthesis. In subsequent experiments, they discovered that lithium interacts with an enzyme IMPA1, suppressing it from catalysing the formation of Inositol, essential for a continuous supply of PIP2 in the cells. When they removed the IMPA1 from a group of cells, it turned out that lithium could not modulate the hyperexcitability of the brain cells.
The next answer the team was keen to find was how lithium decelerated calcium influx. They looked at the expression of genes required to form subunits of voltage-gated calcium channels– protein doors that allow calcium movement through the neural cells. They found that lithium dialed down the functions of genes required to put together different pieces of the calcium channels. They found that several genes essential for the signaling pathways initiated by key neurotransmitters, like glutamate, that regulate calcium influx were also down-regulated.
“In clinical medicine, we often find that not all patients respond to medications available in the market. It will be valuable for doctors to clearly predict which patient will respond to a given medicine to devise a treatment uniquely suited for that individual; this is a very exciting area called precision medicine that is expanding worldwide”, says Raghu Padinjat, Professor, NCBS.
Precision psychiatry seeks to optimize treatments while reducing the burden of unnecessary diagnostic testing and therapies. “The insights from our study into how lithium acts on human brain cells will pave the for lab tests to help doctors predict which bipolar patients will respond to lithium. This advance in precision psychiatry will help patients with bipolar disorder to get the correct treatment sooner and hence improve the quality of life for patients and their families”, adds Raghu.
This paper can be accessed at: Sankhanil Saha, Harini Krishnan, Padinjat Raghu Life Science Alliance Dec 2023, 7 (2) e202302425; DOI: 10.26508/lsa.202302425








0 Comments